In the 1940s, the cartoon detective character Dick Tracy used a wrist watch to not only tell time but also to communicate with police headquarters. Less than a century later smartwatches and similar devices are poised to become the principal means for measuring health and eventually delivering health care.
Four years ago, over 400,000 individuals from every state in the country enrolled in a groundbreaking study to determine whether an Apple Watch could detect atrial fibrillation. The Apple Heart Study, published in The New England Journal of Medicine, notified 2000 participants of an irregular pulse who were then connected to a physician via a telemedicine visit and sent an ECG patch. A third of those with an irregular pulse were found to have atrial fibrillation on subsequent ECG recordings. The entire study required no in-person visits.
This study provides a powerful glimpse of how (1) health will be measured and (2) care delivered in the future. First, digital devices will monitor the health of willing participants continuously, passively, and objectively. This information flowed first to the technology company (in this case, Apple) before going to a medical center for analysis. Second, at least some care will be delivered remotely over those exact same devices. This care was not provided by Apple but by a third-party telemedicine company (American Well or AmWell). In the future, technology companies may charge health care providers “rent” for access to their platforms.
Traditionally, such a study would not even be possible. In person, such a screening study of asymptomatic individuals might require up to 1,000,000 visits. Currently, screening is largely limited to individuals with suspected atrial fibrillation who are often first seen in a hospital and then referred to a cardiologist. After traveling to a clinic, individuals have a single ECG performed at an arbitrary time, are sent home with a Holter or similar cardiac monitor, and then re-evaluated in the office. The monitoring can cost up to $1200, or nearly the price of an Apple phone and smartwatch, and only lasts one to two days.
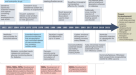
The implications of this transition away from clinics and hospitals are profound (Figure). The first is that the scale and scope of health measurement has increased dramatically. The health of millions of individuals can be and are assessed continuously by an expanding array of devices with increasing capabilities. The utility of these tools is no longer limited to health enthusiasts but can detect early and late signatures of disease as recently demonstrated with COVID-19. Second is the health monitoring can be coupled with health care delivery forming a continuous loop. While such connections are still being developed, companies like Livongo, are using data from web-enabled glucometers to enable health coaches to counsel patients on their diabetes. Such counseling can be synchronous or asynchronous and use artificial intelligence to bypass health care workers altogether. Third, the cost of such measurement and care loops can be orders of magnitude cheaper than traditional care. Expensive visits to physicians or clinics can be reduced or eliminated altogether. Fourth, while a digital divide needs to be bridged, these tools have the potential to provide health care to many who lack such access to health care often simply because of where they live.
Figure. The current and future platforms of health
Coupled with these benefits are significant concerns around privacy, equity and duty. The data captured by digital devices can inform countless aspects of behavior and health. These data could be valuable to marketers, employers, and governments. Just as advances in genetics, especially direct-to-consumer genetic testing, required a Genetic Information Nondiscrimination Act in 2008, the time has arrived for a Data Information Nondiscrimination Act. In addition to minimizing the potential for discrimination, such legislation needs to clearly articulate that these health data belong to individuals who have the right to determine who can (and cannot) see their data and for what purpose.
Current health care is plagued by inequities. Because of their widespread use (the number of smartphone users globally may exceed 6 billion), the digital platforms can help address some of these disparities. But not all individuals have such access. In the U.S., about 20% of households lack broadband access and a similar proportion do not have a smartphone. We need to make broadband access a public good and work to help these technology platforms reduce not exacerbate health differences.
Finally, and most importantly, the owners of these technology platforms are for-profit companies. Their principal duty is not to patients or the public but to shareholders. These shareholders may have different views on privacy and equity than the public or individuals patients. The firms and their owners do not have a duty to patients like clinicians do or a responsibility to act in the public’s interest as non-profits are supposed to do. If their devices will be the new platforms for measuring health and delivering care, the interests of individuals must be protected.
Technology has always shaped medicine. The advent of x-rays and ECGs and advances in transportation in the 1930s drove health care from the home where house calls once dominated to clinics and hospitals. Today, the increasing capabilities of digital devices along with the internet are moving care away from expensive and often unsafe medical centers to homes and mobile devices. This migration will dominate health care for the foreseeable future, holds much promise, and provides potential pitfalls that will require attention from all of us.




Please sign in or register for FREE
If you are a registered user on Research Communities by Springer Nature, please sign in